BACKGROUND
Heart failure is a common condition resulting in severe breathlessness, fatigue and exercise limitation. The most common causes are either related to heart attacks or the dilation and impairment of the cardiac muscle's ability to contract efficently. Some patients suffering from heart failure may develop a tendency to dangerous life threatening arrhythmia and, in rare cases, cardiac arrest.
Traditionally heart failure has been treated with medication, but many other surgical treatment options have now become standard when medication either reaches a ceiling or fails altogether. Identification and treatment of suitable patients with cardiac devices is essential in order to improve the outcome of these patients.
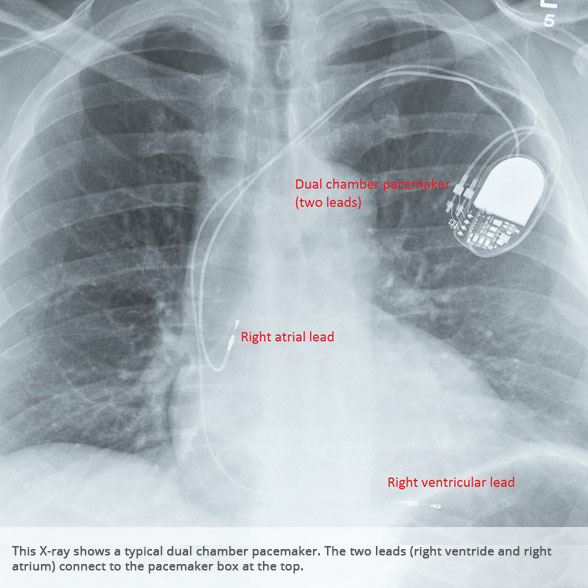
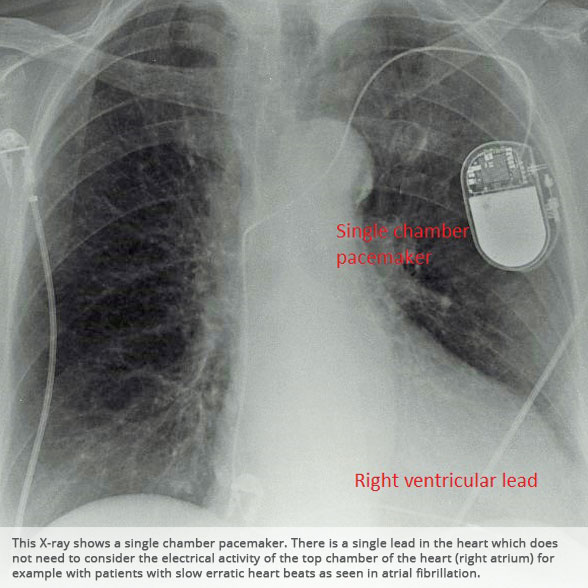
PACEMAKERS
Pacemakers are used mainly to correct slow heart heart rhythms, which can lead to dizzy spells and blackouts. They can be either single or dual chamber devices (one or two leads in the heart respectively). Between 500-600 pacemakers are fitted per year in Gloucestershire.
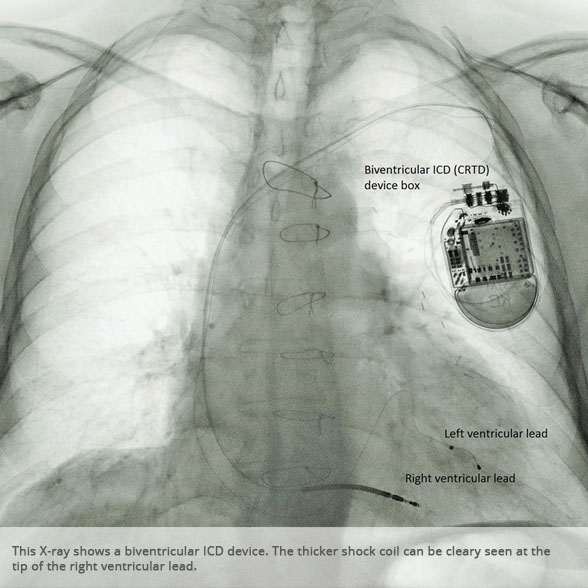
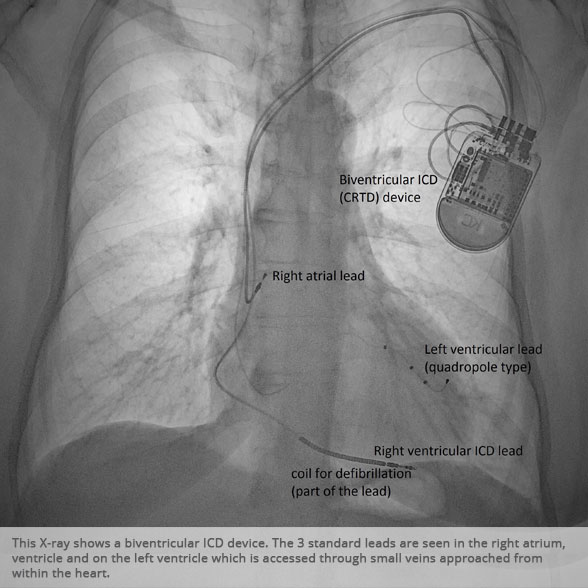
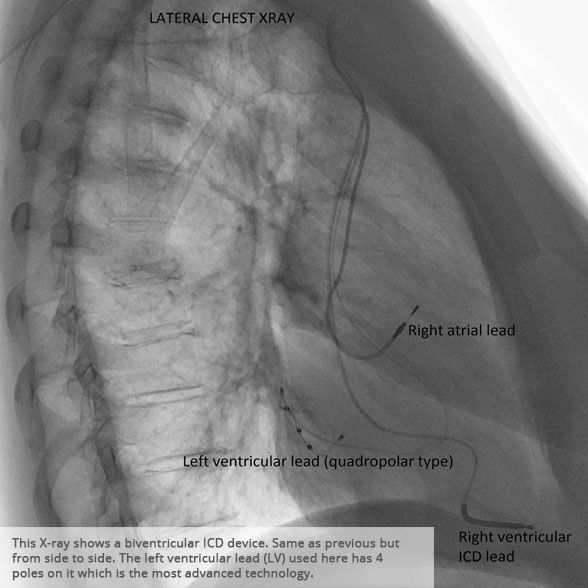
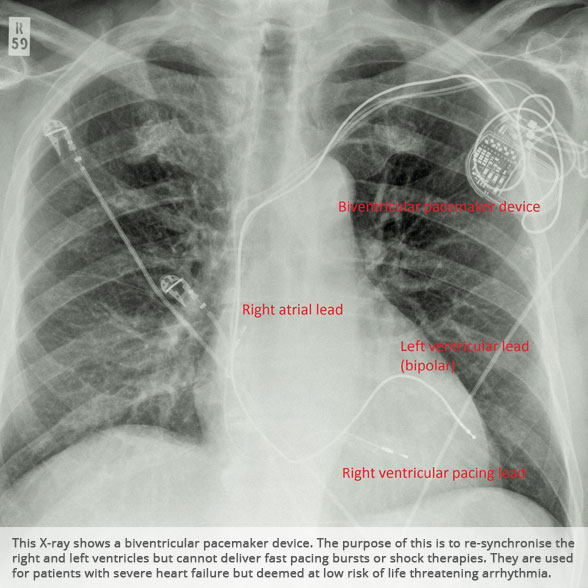
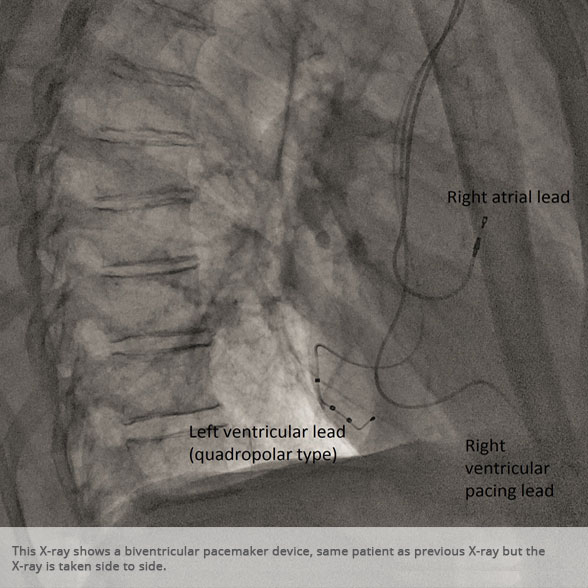
BI-VENTRICULAR PACEMAKERS
Bi-ventricular pacemakers are used for the treatment of suitable patients with heart failure who are already on medication but who suffer from a lack of synchrony between the right and left ventricular contraction. This is most commonly caused by an electrical delay (left bundle branch block LBBB) in transmission of signals to the main pumping chamber (called the left ventricle) and is relatively common in patients with advanced heart failure. This delay process commonly worsens the symptoms of heart failure and it is not generally influenced by medication alone.
Although not all patients universally respond to bi-ventricular pacing (or cardiac resynchronisation therapy/CRT), patients with more advanced dys-synchrony tend to experience remarkable improvement. Bi-ventricular ICDs have the additional benefit of recognising life threatening arrhythmia and deliver both fast pacing bursts or shocks to restore normal heart rhythm.
ICDs
ICDs are used to treat life threatening arrhythmia emerging in the main pumping chambers of the heart (the ventricles). They are offered to patients deemed at risk of such ventricular arrhythmia (primary prevention), for example those who require intervention as a result of significant ventricular scarring after heart attacks, or patients who have been fortunate to survive a cardiac arrest (secondary prevention).
There are established risk stratification algorithms we use to detect patients who may benefit from ICD treatment. ICDs will deliver both fast pacing bursts and shocks to terminate life threatening arrhythmia.